Minimally Invasive Spine Surgery for Lasting Pain Relief
Prone TransPsoas (PTP) lumbar interbody fusion is an advanced form of minimally invasive spine surgery designed to treat conditions such as spinal stenosis, spondylolisthesis, and degenerative disc disease. This modern fusion technique restores spinal alignment, relieves nerve compression, and stabilizes the spine-often with less pain and faster recovery than traditional spine surgery.
PTP allows surgeons to access the lumbar spine through a small lateral incision, minimizing muscle disruption while achieving excellent spinal correction.
What Is Spinal Fusion Surgery?
Spinal fusion surgery permanently joins two or more vertebrae to eliminate painful motion, improve stability, and relieve nerve compression. It is commonly recommended when nonsurgical treatments such as physical therapy, medications, or injections fail to provide lasting relief.
Fusion surgery is frequently used to treat:
- Degenerative disc disease
- Spinal instability
- Spondylolisthesis
- Lumbar spinal stenosis
What Is Prone TransPsoas (PTP) Surgery?
PTP surgery is a minimally invasive lumbar fusion technique that uses a lateral approach to the spine while the patient is positioned prone. This approach allows for:
- Restoration of disc height
- Correction of spinal alignment
- Indirect decompression of spinal nerves
- Reduced muscle injury compared to traditional fusion
By minimizing tissue disruption, PTP often leads to shorter hospital stays and quicker
Conditions Treated With PTP Lumbar Fusion
PTP is particularly effective for common degenerative spine conditions, including:
Spondylolisthesis
A condition where one vertebra slips forward over another, causing instability and nerve compression. PTP stabilizes the spine and restores proper alignment.
Lumbar Spinal Stenosis
Narrowing of the spinal canal or nerve openings that causes leg pain, numbness, or weakness-especially with standing or walking. PTP restores disc height to relieve nerve pressure.
Degenerative Disc Disease
Age-related disc degeneration that leads to disc collapse, instability, and chronic back or leg pain. PTP restores spacing and stability between vertebrae.
Common Symptoms of Lumbar Spine Conditions
Patients who benefit from PTP surgery often experience:
- Chronic lower back pain
- Leg pain (sciatica)
- Numbness or tingling in the legs or feet
- Muscle weakness
- Difficulty standing or walking long distances
- Pain that improves with sitting or leaning forward
Why Does Sitting or Leaning Forward Relieve Pain?
In conditions such as spinal stenosis, sitting or bending forward temporarily opens the space around spinal nerves, reducing compression and improving blood flow. This explains why symptoms worsen with standing or walking and improve when sitting-a pattern known as neurogenic claudication.
Why PTP Is an Effective Solution
PTP surgery addresses the root cause of nerve compression rather than just treating symptoms.
By restoring disc height and spinal alignment, PTP:
- Permanently reopens nerve pathways
- Reduces pressure on spinal nerves
- Stabilizes unstable spinal segments
- Allows patients to stand and walk comfortably without needing to lean forward
Benefits of PTP Minimally Invasive Spine Surgery
Compared to traditional lumbar fusion techniques, PTP offers several advantages:
- Smaller incisions
- Less muscle damage
- Reduced blood loss
- Improved spinal alignment
- Faster recovery and rehabilitation
- Shorter hospital stays
PTP vs Traditional Lumbar Fusion Surgery
How PTP Surgery Is Performed
1. Positioning and Access
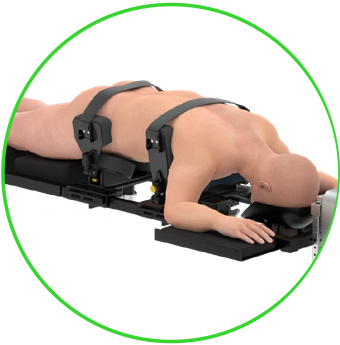
The patient is positioned prone. A small incision is made on the side of the abdomen to access the spine.
2. Disc Removal and Preparation

The damaged disc is removed, and the space is prepared for fusion.
3. Interbody Implant Placement

An interbody spacer restores disc height and alignment. Bone graft is added to promote fusion.
4. Spinal Stabilization
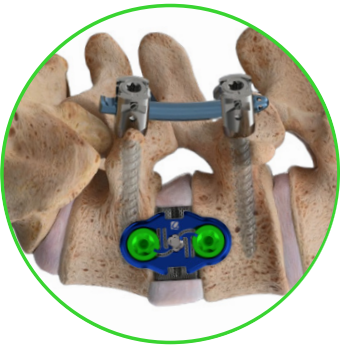
Screws and rods may be placed through small incisions to ensure long-term stability.
Recovery After PTP Surgery
Most patients are encouraged to sit upright and walk soon after surgery.
Typical recovery includes:
- Hospital stay of 1–2 days
- Gradual return to normal activities
- Improvement in leg symptoms early, with continued healing over time
Patients receive individualized instructions regarding:
- Activity restrictions
- Medications
- Wound care
- Physical therapy
Is PTP Right for You?
PTP lumbar fusion is not appropriate for every patient. A thorough evaluation-including imaging, physical examination, and discussion of treatment goals-is essential.
If you suffer from lumbar spinal stenosis, spondylolisthesis, or degenerative disc disease and are seeking a minimally invasive spine surgery option with faster recovery, PTP may be an excellent choice. If interested please reach out through the patient portal and request a consultation.



